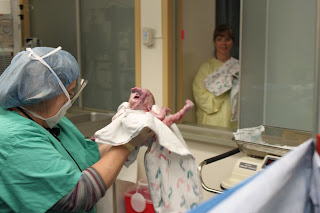
Drew's labs continued to show signs of infection this morning and it was decided that they would perform a lumbar puncture, spinal tap, to examine his spinal fluid for bacteria. They assured us that they would use a local pain med and that because he was so young he wouldn’t remember a thing. They would wait a few hours to perform the procedure. His breathing had been fine during the night so they decided not to administer the surfactant. We were both happy about that. The happiness didn’t last long. Later in the morning the Nurse Practitioner felt that Drew was having a harder time breathing and ordered a chest x-ray. The film showed that there were pockets in the lungs where the alveoli weren’t open. They would want to intubate him for about twenty minutes while they administered the surfactant to each side of the lungs. Our nurse for the day shift told us she thought it would have been better for him to have had the procedure the night before because often times it will help immensely with the babies breathing. Since they don’t want to stress Drew out too much they would postpone the spinal tap till tomorrow. Michelle’s mom came to visit while we waited for them to start. Glenn was on his way in the hospital when they started. They thought it best for us to leave. After it was all complete they allowed Glenn and I to give Drew a blessing. Last night we decided on Drew’s middle name. He will be called Andrew Rawson Cardon. Rawson is my Grandpa Gaisford’s middle name and his mother’s maiden name. We both think it fits. After the blessing we let Drew rest since he had been through a lot. The rest of the night we just sat around.

This morning Drew is breathing better than before. The treatment must have worked yesterday, but he is still on the CPAP. We hope not for much longer. Today they will perform the spinal tap. I know how hard it can be for a practitioner to do a good job on an adult and am scared to think how much harder it is on a baby. We must have confidence in those taking care of Drew and hope that they know what they are doing. While they perform the procedure we will take a break and hang out upstairs in Michelle’s room. When we returned from our break Drew looked peaceful. He only had a small Band-Aid on his back and the nurse said they only had to poke him once. I guess we will just have to believe them. After a few hours Drew’s preliminary CSF results came back. They looked good. The graham stain was negative and there were no white cells in the fluid. We will have to wait another two days before we are sure it is clear for bacteria. Even if there is no infection in his spinal fluid he could still have it somewhere else in the body. You never know what is going to happen. We can just hope for the best. Drew is being a trooper and we know he will be a strong one if he can get past all of this. He has been such a good baby and rarely cries at all. We still can’t believe he is ours. Both of us need our rest, because I have to be up so early Michelle told me to go home and get some good rest. I will just be a few buildings down from her tomorrow at work.


So today was a bad, but very good day. Michelle spent several hours watching while they poked Drew 10 different times to start an IV. Then on top of that some labs improved, but others continued to make them think he might have an infection still somewhere in the body. Because he had bowel loops they thought it could be the beginnings of Necrotizing Enterocolitis, which we do not want. I had tried calling Michelle earlier in the morning, but she didn't want to leave his room to answer the phone. A few hours later she texted me wondering if I was coming to visit, I did during my break. Michelle was a little upset over the whole situation. I returned to work only to be told by my co-workers that I should just leave for the day and I returned to Baby Drew. In just about the 45 minutes I was gone they were less concerned about the infection, decided to remove the CPAP, put him on a nasal canula, insert a PICC line, and begin to start his feedings all throughout the afternoon and evening. To add to the good news, Michelle was discharged from the hospital and we were about to go home for a few hours and eat, thanks to some ward friends, and Michelle took a nap. We are now back with Baby drew for a little while. He is doing really well and at this moment he is laying skin to skin with his mommy in Kangaroo time. He loves it so much. We hope you really enjoy these pictures, because we begin to see his face a little more. He had his eyes open for almost an hour and it was so cute. Thanks for all of your prayers and concerns. We won't complain if they keep coming.


When we got in this morning the nurse said he had done really well during the night. We missed being able to take his temperature and change his diaper, but I was able to hold his syringe while we fed him 7ml of Michelle’s milk. She is a champion pumper. To help him associate this time with real feedings we gave him a binky at the same time. He sucked on it really well and he held my finger almost the whole time. His labs continued to improve this morning so during morning rounds they discussed taking him off of the bilirubin lights and also decreasing his oxygen flow from 4 to 3. After we had lunch the Respiratory Therapist came in to change his oxygen flow down and we stopped his bili lights. During his afternoon feed, he was wide awake and stared at Michelle and I the whole time while we held his little hands. The nurse, Jennifer, was nice enough to take some pictures for us. We loved it and so did he. Tonight while Michelle finished having fun with her friends, I got to do all of his p.m. cares (diaper change, temperature check, feeding gauvage style). It was nice to have some time with him. Later on Michelle came back and he had some labs drawn, but then I was able to have my Kangaroo time with him for an hour. It was great, except for his dried out umbilical cord pressing into me. By the time I was done it was time to do his midnight cares and feeding, he’s up to 11 ml, and then off to bed for me and Michelle. All in all it was a good day.


Today Michelle and I slept in. I actually woke up before her to take care of some bills and finances. I was surprised she could sleep in so long, but it was some much needed rest. We hurried to get ready so we could be there for his noon cares. We made is just in time and the nurse had some really good news for us. He had handled his oxygen really well through the night so they moved the flow from 3 to 2. With that adjustment they decided they could start doing non nutritional breast feedings. That means Michelle would pump first and then have him latch on so that he didn’t get any milk. This helps him adjust to and practice sucking and breathing at the same time and get use to Michelle. His cares went well as usual. He always does better when we are close to him. After his 3pm cares Michelle attempted to do non nutritional feedings. He had been sleeping and didn’t want to latch on. There was a little crying involved, but in the end he just ended up being held. He might not be ready for that just yet. For dinner Michelle and I walked to Costco and got some pizza and then decided to buy a camera since we had been borrowing one from our friends (Matt and Vicki if your reading this we hope to be giving it back this weekend once we exchange the one we just bought today for the better one). When we returned I noticed they had turned his oxygen flow back to 3. He had had some troubles with the level 2 and since it had been a fast transition down felt good about the transition back up. After returning from a break at home we came back for his 9pm cares. He was doing very well and was wide awake. I changed his diaper once again and it was poopy. I always seem to get those ones. His feedings are now up to 16 ml and he’s still holding strong, in fact he is now 1860 grams (about 4 lbs 1 oz) when he was originally just 1790 grams (about 3 lbs. 15 oz) at birth. At this rate he might be a football player. It was hard to leave him, but at least he looked very comfy all wrapped up as we left. I hope he understands that we need our sleep too.


We actually got up in time for his 9 am cares. While Michelle was pumping I took a trip to Costco to return our new camera from yesterday with a different new camera. They gave me a little hassle because Michelle wasn’t present, but none the less I was able to purchase it. After I got back Michelle’s parents stopped by. Michelle was trying to do non nutritional feedings with Drew. She held him like a football and he handled it much better, but still didn’t do much sucking. The nurse practitioner decided that even though he was still on an oxygen flow of 3 she could continue with those feedings and also increase holdings to twice a day. They even discussed moving him out of his incubator and putting him in an open basinet. Michelle was very happy as was I. After a visit with the parents Michelle and I took a lunch break along with Tina, her sister, who was doing some clinicals in the Neuro ICU. We had a great chat. At Drew’s 3 pm cares I was able to dress him in his first outfit. He looked pretty good except for the arm with the PICC line that has to stick out of the clothing. With little time to spare, we then took another break and joined Grandma and Grandpa Woolley, and their friends at the Hale Center Theater. We had bought season tickets with the group and were excited to join in on this tradition that has lasted over 30 years. After the show we went to a diner off of State Street for some dinner. As we returned to the hospital we were glad to see that a basinet was placed next to Drew’s incubator all ready for him to use. He had been bundled up really tight and when we took his temperature he had maintained his temperature quite well. Michelle tried her non nutritional feeding again and Drew was a champ. He was actually sucking this time and it lasted for at least ten minutes. The nurse was both surprised and impressed. We were proud of him. At the same time we fed him his 20 ml of breast milk. He is moving up so fast on his feedings and all of the milk is paying off. When we weighed him tonight he was 1910 grams. That is 4 lbs 3.5 oz. He is getting bigger and bigger every day. By next week he could be five pounds. The best part of the evening was for me to be able to hold him again. The last few days Michelle has been the only one to hold him since he was only given one holding a day. He was very happy to be with daddy. Once again the night came to an end and we had to re-dress him, wrap him up, and place him in his new open basinet. He loved it so much. He had a very good day. We are so proud of his progress.


Michelle tried non nutritive breast feeding again during his 9 am cares. He didn’t take quite as well as last night, but he tried. Later in the morning we were able to take the sacrament just down the hall from the NICU. They have couples called to do this service for both employees and patients/parents. During morning rounds they decided to change his flow from 3 to 2.5, along with that he is now able to be held during each feed. That means if we stayed for 24 hours we could hold him 8 times a day, but we are usually only around for 4 to 5 of those times. It is just great to have the chance to hold him. His temperature continues to hold strong in the open basinet and he is already bigger than some of the preemie clothes they give us to dress him in (length wise that is). His feeds are continuing to increase. By tonight he will be on 26 ml of breast milk and they are also considering changing his fluids from TPN to a regular IV fluid by tomorrow. At this rate he will be on full feeds and off fluids by Tuesday. After his 3 pm cares we went to Rachael’s apartment for dinner and then brought her and Steve back to see Drew. They got to see me in action while I took his temperature, changed his sat probe, changed his diaper, and all of his clothes and blankets. They said I was a pro. Drew’s 9 pm feeding was another try at non nutritive feeding. He seemed a little more tired than usual and just latched on without much sucking. They say this can happen when he has to start using more energy to keep his body temp up. Now that he’s not in the incubator they used a portable scale to weigh him. We were afraid that maybe his weight would go down because the differences in scales, but he surprised us. He is now a whopping 1925 grams (just shy of a full 4 lbs 4 oz). When it was time to feed I got to hold him. We, me and him, liked it very much. At the end of the night, when it was time to go, we put him back in his basinet and his stomach was very, very, very full. So full he had difficulty breathing, but before we left his vitals looked good. The nurse is going to try him on a flow of 2 for his oxygen during the night. We hope he does well. It is hard to leave him at night, but we are amazed at the progress he makes each morning when we return.


This morning the nurse told us that Drew had a little green emesis in two different spit ups. He spit up about 4 ml of his meal after we left last night and had a lot of air in his stomach. They decided to take an x-ray of his stomach, but everything looked good. When the nurse practitioner came by she said they weren’t really worried about it because it looked light in color and milky and everything else looks really good. His non nutritive feeding went about as well as yesterday, a lot of latching on, but only a little sucking. Because of his possible reflex last night they had decided not to move him down to a flow of 2, but this morning during rounds they decided he was ready and as of now he is handling it like a champ. No doubt he’ll be at a 1.5 tomorrow. They also increased his feedings once again. By 6pm he will be getting 31 ml of breast milk which is just over an ounce. They also just brought out his new IV fluid and will take him off of the TPN and lipids later tonight. It looks like he will reach full feeds by tomorrow based off of 150 Kcal per Kilo. Our family friend, Toodie, stopped by the hospital for a short visit. We appreciate everyone’s thoughts and concerns. Drew continues to control his own temperature, all day he has been around 37.2 -.3 degrees Celsius. We may have one too many blankets on him. I am sorry to report that tonight Drew lost weight. He ended up being 1890 grams (4 lbs almost 3 oz), but he working on learning to do a lot of things himself. Michelle had another opportunity to non nutritive breast feed and this time it went great. Before she even started he was trying to put his whole hand in his mouth. He was wide awake and loving it. He kept sucking away for at least 20 minutes. Since we didn’t want him to use too much energy we decided to just let him lay down while he was fed. I have to go into work tomorrow, but hope to be done before his 3pm cares. Then I have another seven days off. I appreciate the support of my work for giving me five days off this past week. I appreciated it and I know Michelle especially has. It will be fun to find out all the changes they might make to his care tomorrow morning. It will be nice to have fewer and smaller tubes coming out of his body. We will see what happens.


While I was at work Michelle kept tabs on baby Drew. He non nutritive breast fed once again like a pro. Maybe he did it so well because he knew it could be his last chance before the real deal. During morning rounds they moved him up to full feeds, 36 ml. That would mean no more IV. They also changed his flow to 1.5 from 2 with a possible change to 1 later in the evening. With the full feeds and the lower flow Michelle was told she could start actually breast feeding. Before any attempts Michelle met me for lunch over at the lab. Later she made two attempts at breast feeding. Both attempts she made weren’t a huge success. He seemed tired, but she still enjoyed holding him. As soon as I was off of work I made my way to the NICU. He really loves his dad a lot and always behaves himself. After his 6pm cares and feeding, and while to NICU was closed for shift change, they took out Drew’s PICC line. He is now free from IV’s and can actually put on his clothes completely. We tried to get the respiratory therapist and nurse to change his flow to 1 and also change to a smaller nasal canula, but the nurse practitioner wanted him to be on 1.5 for at least 12 hours. She had no good explanation for that number, but there was nothing we could do, so that means at midnight tonight they will be changing him to a 1. We asked the nurse to take pictures of him when they changed it so we could see his face without any tubes, except the NG tube. Little by little he is improving each day. The last few nights we have had fun guessing his weight for the night. Tonight I won with a guess of 1905 grams. He turned out to be 1910 grams, up 2/3rds of an ounce from yesterday. He continues to open his eyes more and more during each feed and makes the cutest expressions ever. Michelle has a hard time giving him up when it’s my turn to hold him. We are excited to see him tomorrow. Each new day is a new adventure.